A Novel Approach Using Continuous Monitoring of Peripheral Edema in Heart Failure Patients Allows Recognition of Acute Decompensation Early in the Window of Intervention
Kessler, et al presented a poster session on “A novel approach using continuous monitoring of peripheral edema in heart fialure patients allows recognition of acute decompensation early in the window of intervention” at the HFSA, 2021.
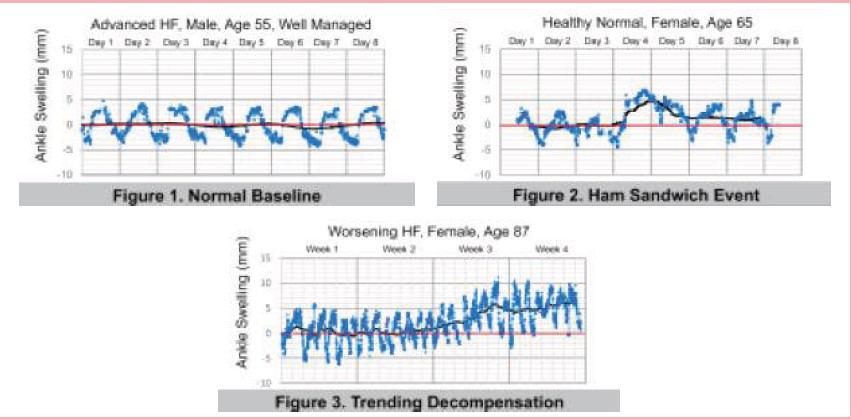
A continuous relaible quantitative measure of peripheral oedemia would provide fluid status that is essential to management of worsening heart failure. It is hypothesized that continuous accurate measurement of ankle circumference can detect decompensation early in the window of intervention. Six male and six female were enrolled for continuous monitoring of ankle circumference for duration of one to six months. The anklet was worn continuously and circumference was measured every 10 minutes; the cumulative orientation was collected every 10 min. The measurement accuracy was 1 mm. The anklet was a comfortable, waterproof devive with a battery life of 4 months.
Continuous monitoring of ankle circumference using the established criteria for accurate and reliable measurements yeilded the following results. The Daily Swelling Pattern (DSP) is correlated with limb orientation. Well-managed heart failure subjects present a DSP and normal baseline substantially equivalent to healthy normal subjects. Fluid retention presents as deviations from the normal baseline.
Quantification of fluid status provides early recognition of decompensation. Ability to detect and interpret ankle swelling patterns provides the opportunity to improve self-care, optimize therapeutic effectiveness, and respond early in the window of intervention to prevent heart failure hospitalizations.
Significantly Reduced Healthcare Costs with Home Furoscix Versus in Hospital IV Diuresis: Results from the FREEDOM-HF Study
Tucker John presented the much awaited results of the FREEDOM-HF study in the session “Significantly reduced healthcare costs with home furoscix versus in hospital IV diuresis: Results from the FREEDOM-HF study” at the HFSA, 2021.
FUROSCIX is an investigational, proprietary furosemide solution formulated to a neutral pH, designed to allow for subcutaneous infusion via a wearable, pre-programmed on-body infusor, for outpatient self-administration. FUROSCIX is being developed for the treatment of congestion caused by fluid overload in adult patients with New York Heart Association (NYHA) Class II and Class III chronic heart failure (HF) who show diminished response to oral diuretics and do not require hospitalization. FUROSCIX, if authorized, has the potential to give an outpatient therapy option for worsening heart failure caused by congestion. FREEDOM-HF was a prospective clinical study that assessed the 30-day heart failure-related and total expenses of treating congestion in chronic HF patients. FUROSCIX, the Company’s investigational product, was administered to patients after they were discharged from the emergency department and compared to a historical comparator group that was managed in the hospital setting.
Comparators were hospitalized for ≤72 hours and drawn from a claims database that was matched to seven factors associated with HF-related hospitalization and severity. Baseline patient characteristics (important matching factors) were comparable between research groups, as was the prevalence of co-morbidities and HF medication usage. The use of FUROSCIX resulted in a statistically significant decrease in 30-day HF-related and total healthcare expenses. The FUROSCIX treated group ($2,920) had $17,753 less HF-related expenditures than the comparison group ($20,673, p-value <0.0001). Similarly, the average 30-day total healthcare expenses in the FUROSCIX-treated group ($7,090) were $30,568 lower than the comparator group ($37,658, p-value<0.0001).
There were no major adverse events (SAEs) associated with the study medication, and there were no deaths or withdrawals from the trial as a result of an SAE. The most frequent adverse effects of FUROSCIX were injection site bruising (29%), pain (29%), and dizziness (13%); all were minor in intensity and none resulted in study withdrawal. The cost of FUROSCIX is not included in this study because it has not yet been established.
HF patients with mild to moderate volume overload (despite oral diuretic use) can be safely discharged from the emergency department with subcutaneous FUROSCIX, enabling outpatient decongestion. FUROSCIX use was associated with statistically significant reduced overall and HF-related healthcare costs through a reduction in HF-related hospitalizations.
A Novel Approach Using Remote Speech Analysis in Chronic Ambulatory Heart Failure Patient Allows Early Detection of Clinical Decompensation Leading to Hospitalization or Unplanned IV Diuretics Treatment- Updated New Data
Amir, et.al gave a poster presentation at the HFSA Annual Scientific Meeting 2021 on the topic, “A novel approach using remote speech analysis in chronic ambulatory heart failure patient allows early detection of clinical decompensation leading to hospitalization or unplanned IV diuretics treatment- updated new data.”
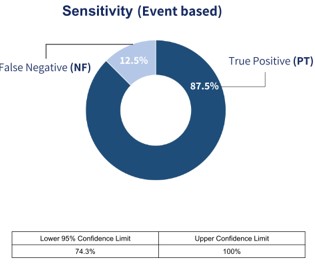
Prevention of acute decompensated heart failure (ADFH) hospitalizations has both medical and economic implications, yet remains an unmet need. Voice analysis may remotely detect the increases in pulmonary and upper airway fluid content. The ongoing multicentre observational study was based on the hypothesis that Cordio HearO™ speech analysis may help in identifying clinical worsening of heart failure (HF) before hospitalization. The study included a total of 180 New York Heart Association Class II-III, stable stage C chronic HF patients. The patients recorded 2-5 sentences each day using Cordio HearO™ operating on standard smartphone devices, collected daily over 29 months. The present analysis explored the association between different speech measures parameters and episodes of HF decompensation requiring hospitalization. A total of 63,901 recording days were there. Of the 24 patients’ HF events, 21 (87.5%) were detected by the system with a mean of 22 days (min: 3 days, max: 31 days) before the HF event. The estimated false positive event rate per year was 2.87, one priority every 4.2 months (approx.) per patient. The system issued a notification 22 days (per patient, on average) before HF-related hospitalization occurred.
Cordio HearO™ novel speech analysis technology may be a useful tool in remote monitoring of HF patients, providing an early warning of impending episodes of decompensation, thus having the potential to reduce ADFH hospitalizations and improve patient quality of life and economic outcomes.
Cordio HearO™ novel speech analysis technology is a useful system for timely detection of clinical decompensation leading to hospitalization. Ongoing and future studies will continue to define the role of speech measures in the management of HF patients.
Which Patients Benefit from Complete Revascularization?
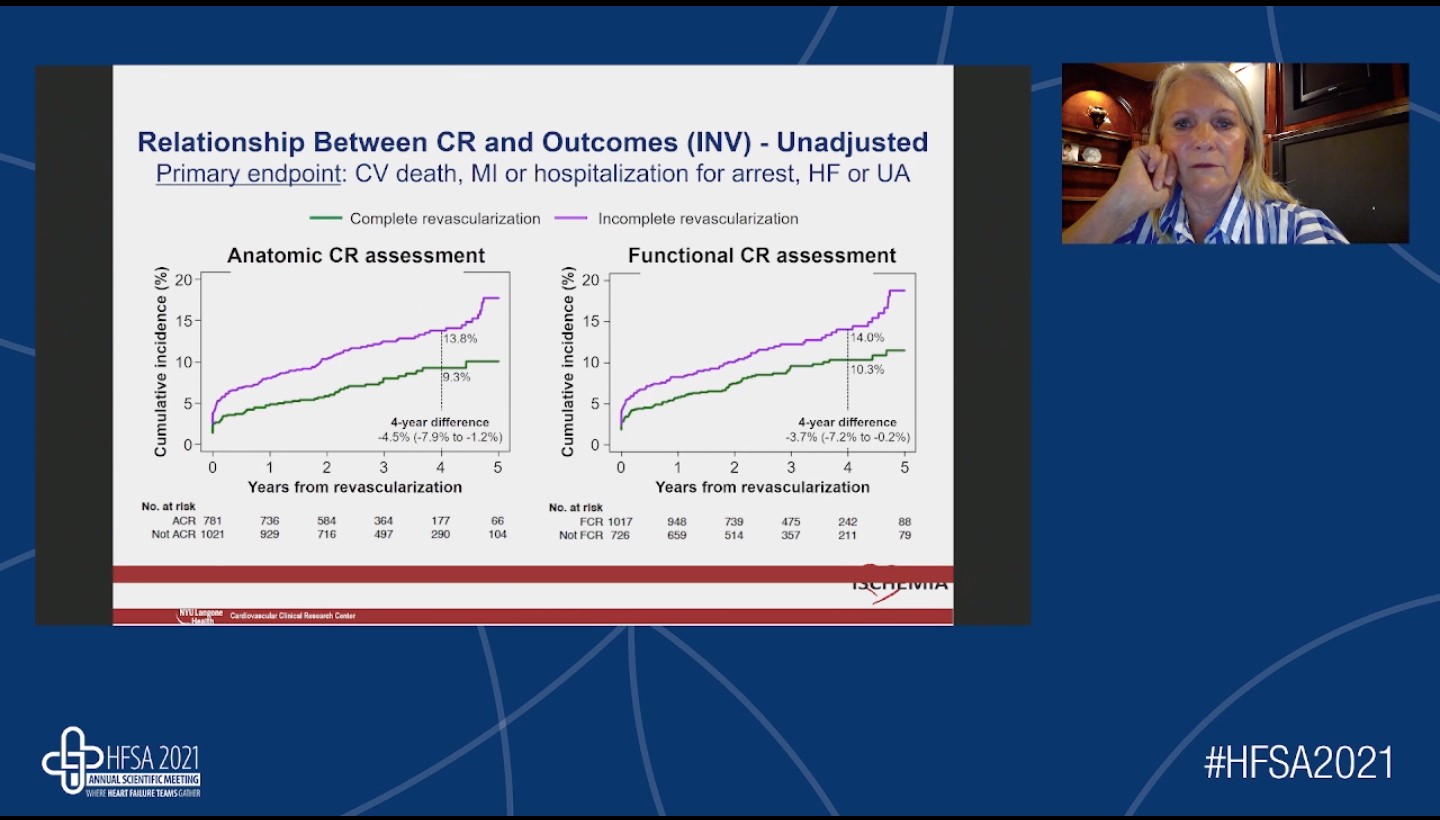
Cindy L. Grines from the Northside Hospital Cardiovascular Institute, Atlanta, Georgia, USA, presented an informative talk on the topic, “Which patients benefit from complete revascularization?” at the HFSA Annual Scientific Meeting 2021. Cindy L. Grines iterated the need for carefully doing risk-benefit assessment in patients with coronary artery disease (CAD). One of the recent studies showed that incomplete revascularization at Index Hospitalization was linked to the higher 1-year death, myocardial infarction (MI), and repeat revascularization. Incomplete revascularization with percutaneous coronary intervention (PCI) is associated with a lower survival rate whereas complete revascularization from either PCI or coronary artery bypass graft (CABG) has similar long-term survival rates. The patients at high risk and complexities have more difficulty in achieving complete revascularization. PCI results in incomplete revascularization than CABG. More extensive revascularization at the Index procedure with Impella support is associated with improved outcomes and risk-reduction in acute kidney injury. According to the results from a very recent SYNTAX Extended Survival Study, incomplete revascularization is common after PCI, and the degree of incompleteness was associated with 10-year mortality. A 2021 R-IMP-IT study revealed that Impella-supported extensive revascularization is associated with lower rates of death, non-fatal MI, and stroke at 1 year. These results are similar to the Roma-Verona Registry study in which more complete revascularization with Impella was linked to increased survival and improved ejection fraction. Cindy L. Grines discussed the findings of The ISCHEMIA Trial in detail. She briefly talked about the study design in which the stable patients with moderate to severe ischemia were randomized to either invasive strategy (optimal medical therapy + catheterization + optimal revascularization) or conservative strategy (optical medical therapy alone).
In 1825 patients randomized to invasive strategy group, 43.3% patients had complete revascularization as per anatomic complete revascularization assessment and 58.3% had complete revascularization as per functional complete revascularization assessment. Complete revascularization was associated with a significantly lower incidence of CV death, MI, or hospitalization for arrest, HF, or UA. Complete revascularization was associated with significantly improved long-term outcomes compared to patients who underwent incomplete revascularization. Complete revascularization had been shown to reduce the risk of all cause death/CV death, risk of major cardiovascular events (MACE), risk of MI in patients with the acute coronary syndrome (ACS), and high-risk ST-elevation myocardial infarction (STEMI).
All patients with significant multivessel disease, in whom complete revascularization can be safely performed will benefit from complete revascularization.
The Heart of the Heart Team

David Wohns, presented an enlightening presentation on the topic, “The Heart of the Heart Team” at the HFSA Annual Scientific Meeting 2021.
The Goal of the heart of the heart team program is to share spectrum health best practices and tools for heart team implementation. The heart team is involved in conducting various diagnostic procedures, percutaneous coronary intervention (PCI) as the patient volume suffering from acute myocardial infarction; high-risk ST-elevation myocardial infarction (STEMI) has increased over the years. Cost, trust and multidisciplinary care are what patient looks for while selecting any health system. The value proposition of the heart team includes efficient decision-making, rapid multidisciplinary input, physician empowerment, and patient empowerment, reduced length of stay, positive outcomes, and team building. Dr. David presented a case of a 67-year old male with severe coronary artery disease and progressive multiple sclerosis-wheel bound. As per the computed tomography (CT) surgery consult, he was a poor surgical candidate. Interventional cardiology consultation confirmed that he was a poor PCI candidate. For such a case, the right approach would be to consider rapid improvement events, present as well as the future state, and evaluate who should do what, when, and where. “Why” a particular procedure to be considered in this case should be communicated clearly. The standard areas to be included are Ad hoc PCI, admission from Cath lab, pre-operative testing/consultation with surgery, outpatient optimization before the surgery, communication with the patient, family, and nursing.
The program, “the heart of the heart team” could provide a comprehensive patient presentation, would encourage discussion, communication, and education, and would help in reaching general consensus/recommendations, and helps in establishing a good physician-patient relationship.
Outcomes in Patients On Chronic Inotropic Support Who Are Not Candidates for Advanced Heart Failure Therapies
Sami F, presented a session on the topic “Outcomes in Patients On Chronic Inotropic Support Who Are Not Candidates for Advanced Heart Failure Therapies” at the HFSA, 2021. She aimed to study clinical outcomes in these patients discharged on inotropes while comparing the dobutamine and milrinone cohorts.
In heart failure patients, guideline directed therapy (GDMT) and device implantation have improved outcomes in heart failure patients. There is no proper study which studied the impact of GDMT and device implantation on patients with advanced heart failure, who are not candidates for left ventricular assist device (LVAD) or heart transplant (HT).
A retrospective multi-center study from Jan 2015 to May 2019 was conducted which included 249 patients, hospitalized with refractory stage-D heart failure and discharged on continuous long-term milrinone or dobutamine therapy. Exclusion criteria consisted of patients on who were candidates for HT or LVAD and those discharged on comfort measures.
In this study, overall age of of patients was 64.8 ±13.4 years and majority of them were males. Dobutamine group had 118 patients and milrinone was used in 131 patients. In both the groups, age and baseline comorbidities were similar with more prevalence in dobutamine group (59.4 vs 52.0; p=0.02). Patients on dobutamine had higher baseline cardiac indices than milrinone group (Fick 2.0 vs 1.8; p=0.048, Thermodilution 2.0 vs 1.6; p=0.002). Patients on milrinone had lower 1-year-mortality compared to dobutamine group (58.1% vs 85.0%; p<0.01).
Milrinone cohort had more patients discharged on beta blocker (42.9 vs 8.6; p<0.001). Other GDMT was also more common on discharge in milrinone group, though statistical significance was not reached.
Mortality is found to be high in in patients started on chronic inotropes who are not candidates for LVAD/HT. Better patient outcomes are observed with Milrinone as compared to Dobutamine.
Time to Decongestion Following Heart Failure Hospitalization as Measured by Extracellular Fluid Nadir Using Bioimpedance Spectroscopy (BIS)
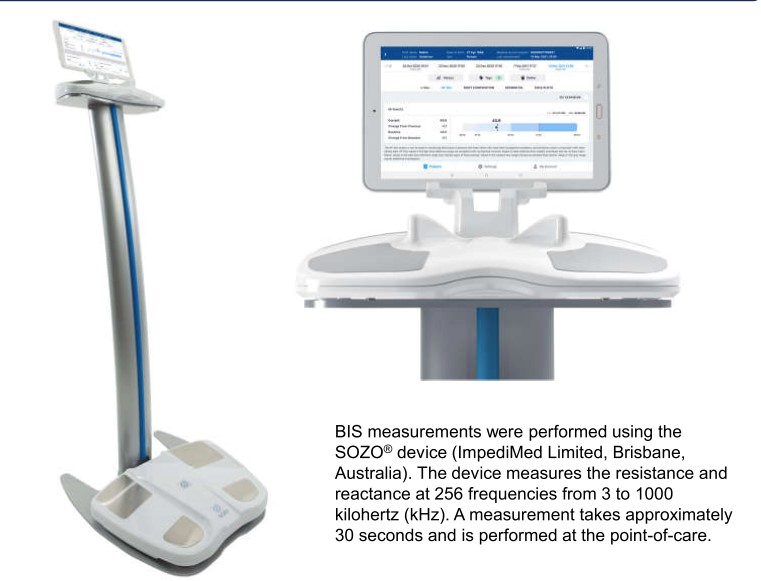
Daleiden-Burns A, presented the poster session on “Time to decongestion following heart failure hospitalization as measured by extracellular fluid nadir using bioimpedance spectroscopy (BIS)” at the HFSA, 2021. This study evaluated daily SOZO® Digital Health Platform BIS measurements using ImpediMed’s HF-Dex™ heart failure index to track fluid status and compared these measurements to corresponding weight measurements.
The SOZO fluid analysis for heart failure provides an objective measurement of fluid volume in individuals with heart failure. It makes use of ImpediMed’s HF-DexTM heart failure index to assist doctors in determining the appropriate fluid volume range for their patients. HF-Dex is based on BIS-derived reference ranges that show normal fluid volumes and high fluid volumes that may necessitate additional clinical evaluation.
Following a heart failure-related hospital stay, individuals had their lowest extracellular fluid volume on average after 16.9 days. Patients lost a median of 7.8 % of their extracellular fluid (ECF) volume versus only 3.4 % of their weight over this period, a statistically significant difference (p<0.0001). The poster indicated that regular monitoring of ECF using BIS measures is a more sensitive technique of monitoring fluid status in patients with heart failure than weight.
The study results demonstrate that non-invasive bioimpedance spectroscopy measurements during the weeks following heart failure hospitalization may assist clinicians in tracking the fluid status of heart failure patients. Monitoring extracellular fluid volume during the weeks after heart failure hospitalization may provide a more accurate measure of fluid status in heart failure patients than measuring weight alone.
Linear Association of Body Mass Index and Mortality in Cardiogenic Shock: A Retrospective Analysis
Delfiner M presented a session on the topic “Linear Association of Body Mass Index and Mortality in Cardiogenic Shock: A Retrospective Analysis” at the HFSA, 2021. He aimed to determine if the BMI correlates with cardiogenic shock mortality.
Cardiogenic shock (CS) continues to have high mortality despite advancements in care, including the development of shock teams and standardized protocols. Obesity is highly prevalent across the world and is a risk factor for overall cardiovascular disease. Obesity has not made its way into common risk assessment platforms of CS. Awareness of a potential correlation may improve risk assessment and inform care plans for CS patients.
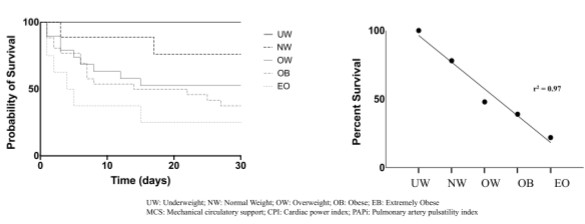
A retrospective analysis of 92 patients from 2014 to 2019 were cared for by a single quaternary care shock team. The shock team comprised of an advanced heart failure physician, a cardiac intensivist, an interventional cardiologist, and a cardiothoracic surgeon. Each patient was subdivided into cohorts: underweight (BMI < 20 kg/m2) normal weight (BMI between 20 kg/m2 and 25 kg/m2), overweight (BMI between 25 kg/m2 and 30 kg/m2), obese (BMI between 30 kg/m2 and 40 kg/m2), and extremely obese ((BMI greater than 40 kg/m2).
The mean age of patients was 62.0 years (SD 12.3 years) and 35 patients (43%) were female. The mean BMI for the total population was 31.1 kg/m2 (SD 8 kg/m2). The mean BMI of patients who survived was 29.7 kg/m2 (SD 8 kg/m2), compared to 33.7 kg/m2 (SD 7.6 kg/m2) for those that did not survive (p = 0.04).
As per this study, an inverse linear relationship between BMI and survival in CS. It has been observed in epidemiological studies that acute coronary syndrome (ACS) related CS yields higher mortality than non-ACS related CS.
Higher BMI is an incremental risk factor for CS mortality and further studies are required that include larger sizes and the measurement of novel biomarkers for obesity and CS.
New York Heart Association Functional Class and Mortality in Obstructive Hypertrophic Cardiomyopathy
Lakdawala N presented a session on the topic, “New York Heart Association Functional Class and Mortality in Obstructive Hypertrophic Cardiomyopathy” at the HFSA, 2021 on the topic. He aimed to assess the associations between NYHA functional class and mortality among patients with oHCM.
Hypertrophic cardiomyopathy (HCM) is a primary myocardial disorder with complex pathophysiology. About two-third of patients with HCM have left ventricular outflow tract (LVOT) obstruction present at rest or with provocation (i.e., obstructive HCM [oHCM]). To assess symptoms and functional limitations among patients with HCM, the New York Heart Association (NYHA) functional class is commonly used.
The study used the data from the Sarcomeric Human Cardiomyopathy Registry (SHaRe), an international registry representing patients from ten HCM specialty centres, up to March 2019. The study cohort consisted of adults with oHCM at least one definite assessment of NYHA functional class. The outcomes were all-cause mortality at 1 year.
In this study, a total of 2495 adult patients had oHCM and at least one definite or indefinite NYHA functional class assessment. On the index date, 38%, 41%, and 21% of patients had NYHA functional classes I, II, and III/IV, respectively. Patients with NYHA functional class I were younger at HCM diagnosis (44 years) compared with class II (49 years) and class III/IV (51 years).
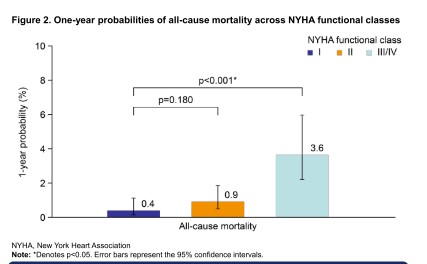
26 patients had died (3 in NYHA functional class I, 8 in class II, and 15 in class III/IV) by the end of 1 year and the risks of mortality increased with worse NYHA functional class. The 1-year probabilities of all-cause mortality were 0.4%, 0.9%, and 3.6% for NYHA functional classes I, II, and III/IV, respectively.
Increased all-cause mortality is associated with worse NYHA functional class in oHCM and proper monitoring of NYHA functional status may improve prognosis.
Do all patients with New-onset Heart Failure need assessments for CAD?
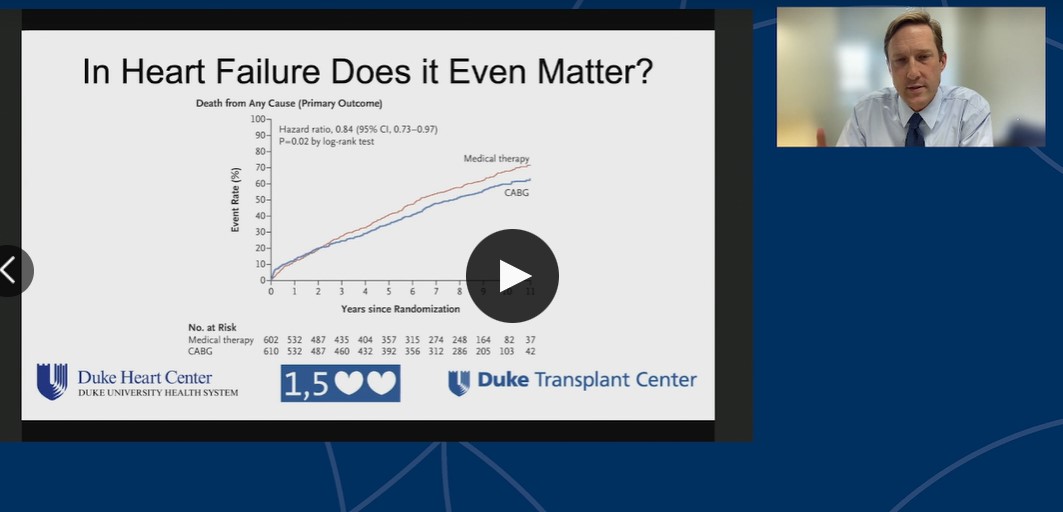
Devore A gave an enlightening presentation at the HFSA, 2021 on the topic, “Do all patients with New-onset Heart Failure need assessments for CAD?” He aimed to discuss the observational data on assessments for CAD and recommend assessments for CAD as quality measure in HF care.
In routine practice, improvements in LVEF are common In CHAMP-HF among 2913 patients with HFrEF, increase in LVEF over time were common over a median of 16 months. He presented a case of 61-year-old male with HFrEF and dilated cardiomyopathy. He was diagnosed with HF and AF 15 years ago and treated with ACEi, BB and MRA. He recently presented to hospital with the episode of acute HF. He arrived on milrinone and intra-aortic balloon pump as choice of treatment. He had a poor urine output despite escalating diuretics and inotropes and impella 5.5 was placed with improvement in end organ function. He underwent transplant at the end of August.
It has been observed that there is underutilization of coronary artery disease testing among patients hospitalized with new onset HF. Testing for HF among patients hospitalized for new-onset HF was 18% which increased to 27% at 90 days after admission
Medical therapy for CAD is a unique therapeutic way for patients with HF and limited testing of CAD can result in missed opportunity to identify appropriate candidates for revascularization.
New-onset HF assessment should be higher than clinical practice and standardized approaches may improve outcomes.

