The American Psychiatric Association Practice Guideline for The Treatment of Patients with Schizophrenia
Assessment and Treatment Plan
Recommendation
APA recommends that the initial assessment of a patient with a possible psychotic disorder include the reason the individual is presenting for evaluation, the patient’s goals and preferences for treatment, a review of psychiatric symptoms and trauma history, an assessment of tobacco use and other substance use, a psychiatric treatment history, an assessment of physical health, an assessment of psychosocial and cultural factors, a mental status examination including cognitive assessment, and an assessment of risk of suicide and aggressive behaviors, as outlined in APA’s Practice Guidelines for the Psychiatric Evaluation of Adults.
The value of psychiatric assessment should not be overlooked because it serves as the initial basis for a patient-related therapeutic relationship and offers information that is important for differential diagnosis, joint care decision-making, and informing patients and family members about factors such as course and prognosis of disease.
Table 1. Recommended aspects of the initial psychiatric evaluation adapted from APA’s Practice Guidelines for the Psychiatric Evaluation of Adults
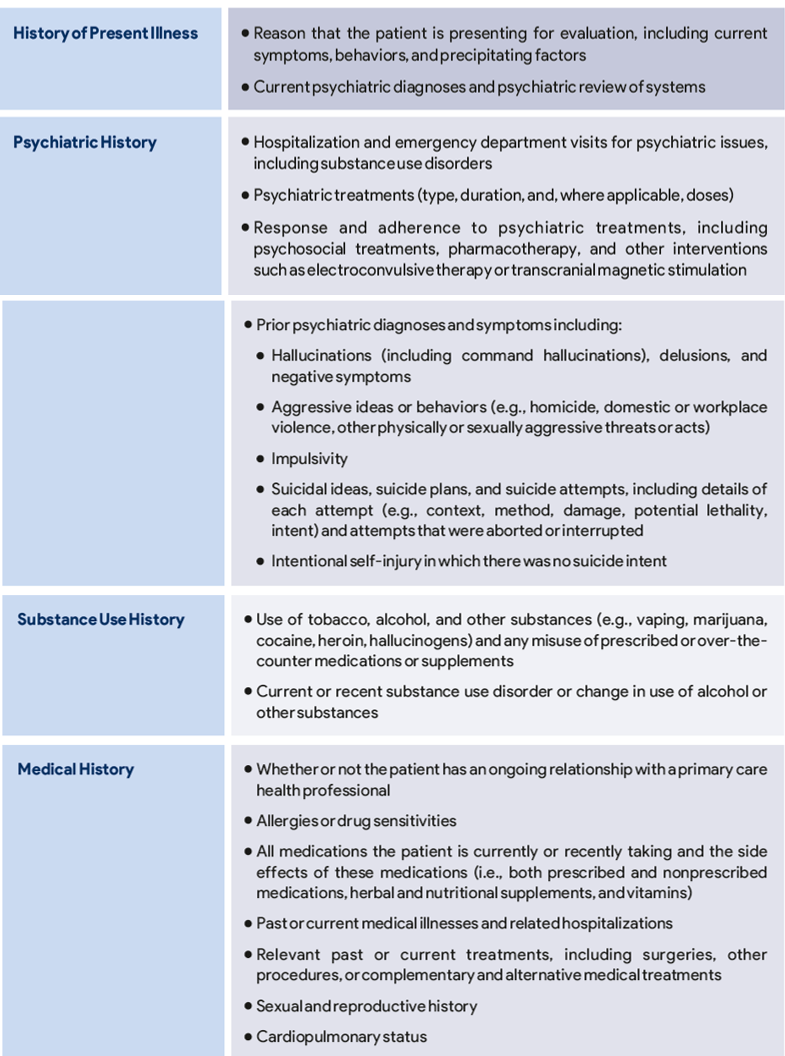
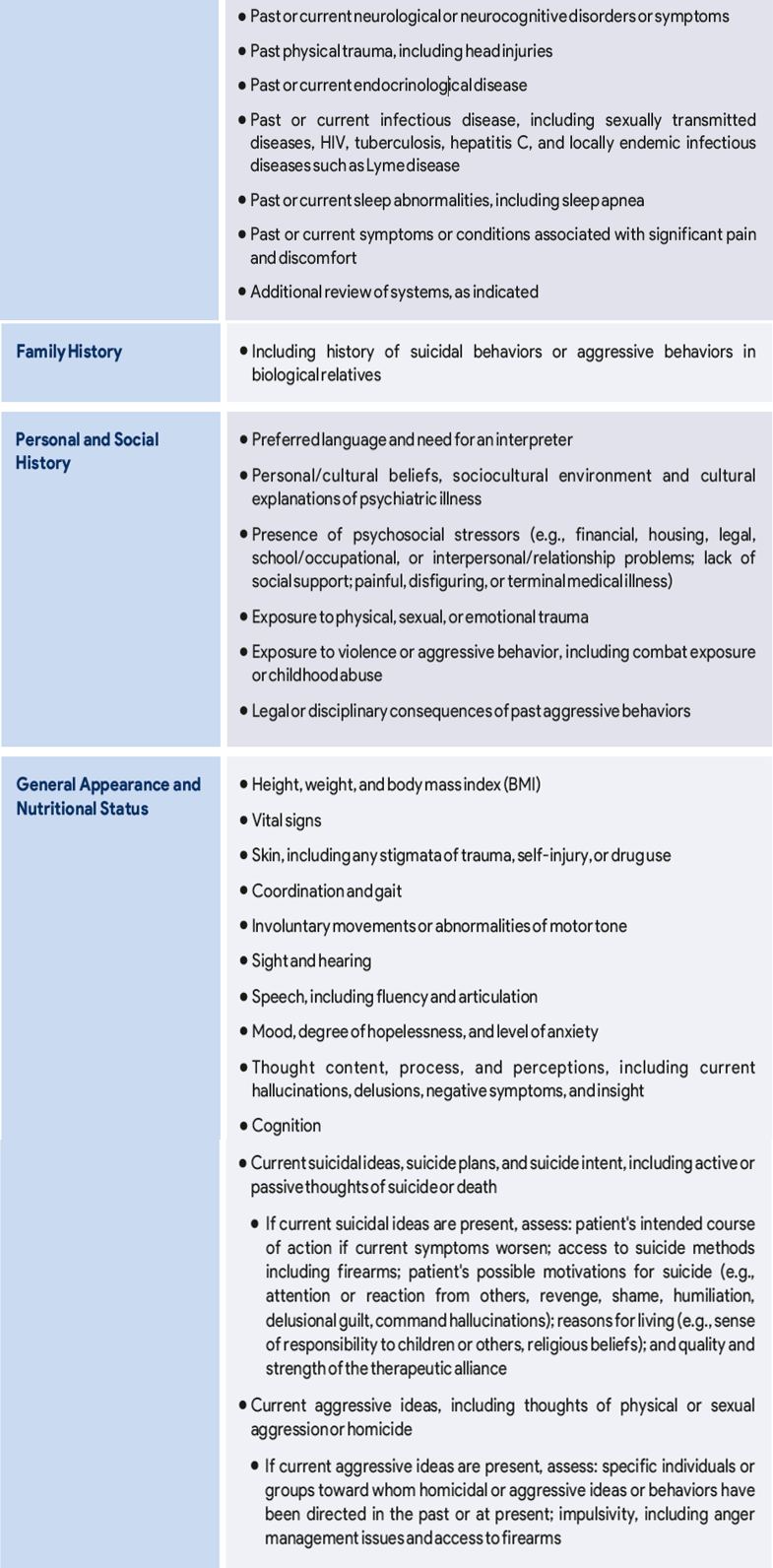
As part of the initial assessment, laboratory testing and physical examination can help classify common co-occurring disorders and can serve as a basis for subsequent monitoring during treatment.
Table 2: Suggested physical and laboratory assessments for patients with schizophrenia
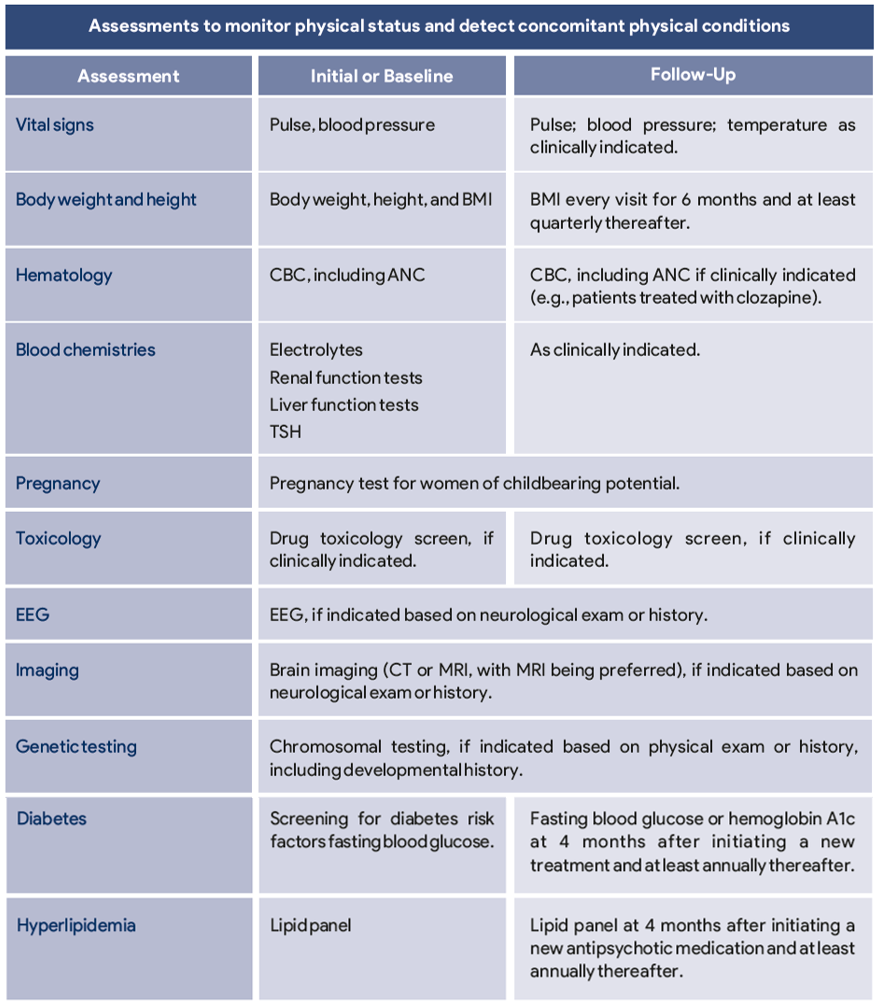
AIMS=Abnormal Involuntary Movement Scale; ANC= absolute neutrophil count; BMI=body mass index; CBC=complete blood count; CT=computed tomography; DISCUS=Dyskinesia Identification System -Condensed User Scale; ECG=electrocardiography; EEG=electroencephalogram; MRI=magnetic resonance imaging; QTc=corrected QT interval; TSH=thyroid stimulating hormone
Recommendation
APA recommends that the initial psychiatric evaluation of a patient with a possible psychotic disorder include a quantitative measure to identify and determine the severity of symptoms and impairments of functioning that may be a focus of treatment.
Quantitative tests can also be used to help detect and evaluate the nature of psychosis and related symptoms in the evaluation of a patient with a potential psychotic illness. The aim of using a quantitative measure is not to create a diagnosis, but rather to supplement the screening and evaluation process with other aspects. It can help in treatment planning, depending on the measure, by having a standardised, replicable way of recording the baseline symptoms of the patient. It may also help to assess which symptoms, based on factors such as frequency of incidence, severity, potential for associated harm to the patient or others and associated patient distress, should be the focus of intervention. The use of quantitative indicators allows for more accurate monitoring, as care progresses, of whether non-pharmacological and pharmacological therapies have the desired effect or whether a change in the treatment plan is necessary. This record of a patient’s reaction to treatment is of special importance when treatment is either non-standard (e.g., antipsychotic combination) or costly. It may also provide valuable information on the real impacts of past therapies. In addition, to explain the longitudinal trajectory of the patient’s condition, patient ratings may be correlated with family members’ experiences of treatment results.
Recommendation
APA recommends that patients with schizophrenia have a documented, comprehensive, and person-centered treatment plan that includes evidence-based non-pharmacological and pharmacological treatments.
A person-centered treatment plan should be established for the treatment of individuals with schizophrenia, recorded in the medical record, and revised at regular intervals with the patient. As part of an appraisal report or progress note, a person-centered treatment plan may be documented and does not need to conform to a predetermined development process (e.g., face-to-face multidisciplinary team meeting) or format (e.g., expectations and goals stated in time).
The initial treatment plan will need to be extended over multiple visits, depending on the urgency of the initial clinical presentation, the availability of test results, and other sources of information, as more history and treatment response specifics are collected. As treatment continues, iterative re-evaluation and improvement may be needed in the treatment plan, triggered by factors such as insufficient treatment response, tolerability or adherence difficulties, insight impairments, changes in presenting issues or symptoms, or revisions in diagnosis. Tailoring the treatment plan based on sociocultural or demographic factors with the goal of improving the quality of life or aspects of functioning (e.g. social, academic, occupational) may also be necessary in adjusting treatment to the needs of the individual patient. Factors affecting the metabolism of medicines (e.g. age, gender, body weight, kidney or liver function, smoking status, use of multiple concomitant medicines) can also require changes to the treatment plan, either in terms of the traditional treatment plan or either in terms of typical medication doses or frequency of monitoring. It is impossible for most people with schizophrenia to put together a coherent picture of the longitudinal course of the patient from medical records. Therefore it is important to remember the reason for any improvements in the treatment plan as well as the specific changes being made, as a key component of future treatment planning is an accurate history of past and current interventions and responses to them.
Pharmacotherapy
Recommendation
APA recommends that patients with schizophrenia be treated with an antipsychotic medication and monitored for effectiveness and side effects.
Selection of an Antipsychotic Medication
The selection of an antipsychotic agent depends on several variables that are peculiar to an individual patient. Therefore, it is recommended that the treating clinician obtain information on the patient’s treatment-related preferences and previous treatment reactions before beginning treatment with antipsychotic medication and then negotiate with the patient the possible advantages and disadvantages of medication as part of the selection of a medication compared to other management choices. In the treatment of schizophrenia, the use of antipsychotic medication may improve the positive and negative symptoms of psychosis and may also contribute to decreases in depression and improve the quality of life and work. The meta-analysis of double-blind, randomised placebo-controlled studies indicated a medium overall efficacy effect size with the greatest effect on positive symptoms. In those who got a response, the rates of obtaining any response or a successful response were also significantly greater. In those who obtained an antipsychotic prescription, the rates of receiving some response or a successful response were also considerably higher. Furthermore, in those hospitalised with antipsychotic drugs, the proportion of individuals who fell out of care for some cause and for lack of effectiveness was substantially lower.
Factors Influencing Choice of an Antipsychotic Medication
Available Drug Formulations
For patients who have trouble swallowing pills or who are ambivalent about drugs and inconsistent in swallowing them, drug choice may be affected by available formulations of particular medications such as oral concentrates or fast dissolving tablets.
Drug-drug Interactions and Metabolism
It is important to pay careful attention to the potential for antipsychotic agents to interfere with other prescribed medicines. For example, side effects (e.g., sedation, anticholinergic effects) can be additive when administering several drugs. In addition, drug interactions may affect the quantity of free drugs available to act on receptors in the blood. Since most antipsychotic drugs are tightly bound to plasma proteins, it is possible to add other protein-bound medicines to displace drug molecules from proteins, leading to a higher percentage of unbound drugs in the blood.
Pharmacokinetic Properties
The absorption of some antipsychotic medications is affected by the presence of food in the stomach. Some individuals may have difficulty in adhering to appropriate meal size or content, which could influence choice of these medications.
Initiation of Treatment with an Antipsychotic Medication
The initial purpose of acute antipsychotic drug therapy is to alleviate acute symptoms in order to get the person back to their baseline level of functioning. Subsequently, maintenance therapy will seek to avoid symptom recurrence and maximise function and quality of life.
Strategies to Address Initial Non-response or Partial Response to Antipsychotic Treatment
A clozapine trial is recommended if a patient has had a marginal or no reaction to two tests of antipsychotic medication lasting two to four weeks at an appropriate dose. A clozapine study is also recommended in patients with a persistent risk of suicide who have not responded to other treatments, and in patients with a persistent risk of violent behaviour who have not responded to other treatments. A clozapine trial can also be suitable in people who have a response to therapy (i.e. have a decrease in symptoms of more than 20 %) but still have severe symptoms or impairments in functioning. In fact, clozapine is frequently underused and many patients may benefit from early consideration of initiation of clozapine. Augmentation therapy can also be considered, but multiple attempts at augmentation therapy may not prolong a trial of clozapine. Particularly for patients with negative symptoms or depression, augmentation of antipsychotic therapy with an antidepressant medication may also be helpful.
Recommendation
APA recommends that patients with schizophrenia whose symptoms have improved with an antipsychotic medication continue to be treated with an antipsychotic medication.
For individuals with a diagnosis of schizophrenia whose symptoms have improved with an antipsychotic medication, there are a number of benefits to maintenance treatment including reduced risks of relapse and rehospitalisation.
Recommendation
APA suggests that patients with schizophrenia whose symptoms have improved with an antipsychotic medication continue to be treated with the same antipsychotic medication.
Usage of an antipsychotic drug that has already been related to symptom response will sustain symptom recovery and encourage better functioning and quality of life. In comparison, improvements in antipsychotic care can be correlated with discontinuation of early treatment, symptom rises, psychiatric destabilisation, and deteriorating tolerability of treatment. Depending on whether the patient develops any serious side effects from the drug that may have long-term untoward effects, the harms of continuing use of the same antipsychotic medication can vary. Continuation of the same drug may lead to greater long-term complications, such as metabolic symptoms or antipsychotic syndromes, but this will depend on the medication’s side effect profile. In some instances, changing to a different medication could worsen long-term side effect risk rather than reduce such risks.
Recommendation
APA recommends (1B) that patients with treatment-resistant schizophrenia be treated with clozapine.
Initiation of Treatment with Clozapine
Clozapine is prescribed for people with treatment-resistant schizophrenia, but the concepts of treatment-resistant schizophrenia in clinical trials and in practise differ considerably. The clinician should include the patient in conversations about clozapine therapy after a patient is diagnosed as having treatment-resistant schizophrenia.
A clozapine trial may also be suitable in patients who demonstrate a reaction to medication (i.e. have a decrease in symptoms by more than 20 %) but still have severe symptoms or impairments in functioning. In fact, clozapine is frequently underused, and earlier consideration of clozapine initiation would help many patients. Discussion of clozapine should underline the values of joint decision-making; it is also helpful to include family members or other support persons in such discussions. In terms of the rehabilitation goals of a patient, most people appreciate the ability to think more clearly and avoid hallucinations or delusions when deciding on changes in medication. In addition, most patients who receive clozapine view it positively.
For example, a broad study of people who were taking antipsychotic medication with schizophrenia or schizoaffective disorder showed that the vast majority of those taking clozapine adhered to therapy and found it beneficial, while only about 5 % found it was not helpful. Many other antipsychotic drugs, on the other hand, were less favourably regarded. Nonetheless, it is necessary to recognise and answer patient concerns about clozapine to the extent possible. For example, patients may express concerns about the burdens of required blood work and may encounter logistical barriers such as transportation. However, they may be willing to consider clozapine if logistical barriers can be overcome or if given the information that blood-monitoring requirements become less frequent over time. Concerns about other side effects, such as weight gain or somnolence, may also contribute to a reluctance to switch to clozapine. Open discussion of these side effects can be helpful with a well-defined plan for monitoring as treatment proceeds. Peer-run support groups that directly address living with side effects can help patients develop strategies for coping with side effects.
Clinicians may also be worried about clozapine, which may act as a treatment barrier. Many physicians, for example, have little experience using clozapine and often raise concerns about paperwork pressures, tracking patient adherence, and side effects of clozapine. Many clinicians overestimate the risk of serious neutropenia and they are hesitant to start clozapine on an outpatient basis. Training on the use of clozapine and its side effects can be effective in overcoming the drug obstacles associated with clinicians. In order to reduce the risks of seizure, orthostatic hypotension and prolonged sedation, slow dose titration is necessary when starting treatment with clozapine. Major rapid increases in the dosage of clozapine have led to cardiovascular failure and death, particularly in patients taking prescriptions for respiratory depressants such as benzodiazepines. From a starting dose of 12.5 mg once or twice daily, the daily dose of clozapine can be increased by, at most, 25 mg to 50 mg per day to a target dose of 300 mg to 450 mg per day. Subsequent dose increases, if needed, should be of 100 mg or less, once or twice weekly. Although efficacy is often seen at a dose of 300 to 450 mg per day, some individuals may need higher dosages of clozapine, to a maximum daily dose of 900 mg, for full response. For patients with an initial episode of schizophrenia and others who are older, significantly impaired, or vulnerable to side effects, a slower rate of titration may be needed. Those with a pre-existing disease of the central nervous system, like those with deletion syndrome, often warrant a slower titration rate and may have an elevated risk of seizures at normal doses.
During initial dose titration, the use of divided doses can be effective in mitigating side effects, but many patients are eventually treated with a single dose at bedtime to reduce daytime sedation and encourage adherence. Throughout the dose titration process, monitoring for therapeutic benefits and side effects of clozapine should occur. Since clozapine titration progresses slowly, there may be no immediate notice of the therapeutic benefits and side effects may be more prevalent than benefits. Therefore, educating and reassuring patients about the anticipated timeline for the therapeutic effects of clozapine may be beneficial. If clozapine is resumed after a 48-hour or longer treatment gap, it should be resumed once or twice daily at 12.5 mg. If this dosage is well tolerated, the dose can be increased more rapidly to the therapeutic range than indicated for initial therapy. It is better to taper the dosage if a decision is taken to quit clozapine, unless the drug is being stopped for medically urgent reasons.
Use of Clozapine Levels During Treatment with Clozapine
While the dose of clozapine is being titrated, blood levels of clozapine and its main active metabolite, norclozapine, should be collected. If there are concerns about medication adherence, less effectiveness or more side effects than expected, possible drug reactions, or other factors that can affect clozapine levels, blood levels may also be helpful. Although there is considerable variance between individuals, the level of clozapine at a given dose will normally be higher in non-smokers than in smokers, in heavy caffeine users than in non-users, in women than in men, and in older individuals than in younger individuals.
In addition, the change between different generic types of clozapine can lead to a difference in blood levels of 5 %-10 %. Clozapine levels should be drawn at the steady state (three days or more after the adjustment in dose) and at the dosage level at the trough (approximately 12 hours after the last dose). Usually, patients will receive a dose of clozapine at bedtime and then have their dose taken the next morning before the additional dose is given. There is not an absolute level of clozapine that is associated with either efficacy or toxicity. Efficacy at levels greater than 350 ng/ml of clozapine would be highest in most patients, although some patients will demonstrate responsiveness or relapse prevention at levels as low as 200 ng/ml. With clozapine levels in the blood, the risk of having seizures increases. As with the findings of every laboratory examination, the clinical context should be considered for the interpretation of clozapine levels. For example, if the dosage of clozapine is much higher than expected, evaluate for side effects associated with the dose and clinical evidence of toxicity.
Optimize Treatment with Clozapine
While studies indicate that at least one-third of people with treatment-resistant schizophrenia will respond to clozapine, there will be no full response in some patients. It is necessary to ensure that an appropriate target dose (typically 300 to 450 mg per day has been achieved before determining that a patient has not responded to clozapine and that steady-state clozapine and norclozapine levels appear to be sufficient to provide a therapeutic benefit. Although no absolute level of clozapine is associated with efficacy, if no response is evident and clozapine is well-tolerated, the clozapine dose should be increased to achieve a clozapine level of greater than 350 ng/ml. In general, to assess reaction, this dosage of medication should be maintained for at least eight weeks, while more dose increases can also be made, if tolerated. If, as for any patient treated with clozapine, no evidence of benefit appears to exist, the value of the drug should be regularly measured in terms of the patient’s reaction, the side effects of the medication and the availability of any potential treatment options. It may be helpful to use a quantitative measure longitudinally in assessing functioning and overall response and identifying specific symptoms that have or have not responded to treatment.
Continue Clozapine and Augment with Another Medication
The evidence basis for other therapies for individuals who do not respond to clozapine alone is limited, although a variety of alternatives have been attempted. Increased use of clozapine with another drug showed no substantial benefit in double-blind research, although some benefit was found in open label studies and meta-analyses of relatively low-quality studies. Increases in other antipsychotic medicines (FGAs and SGAs), anticonvulsants, and other drugs have been investigated. When an augmentation therapy trial is performed, the possible additive effects of the drugs on side effects and the potential for drug-drug interactions should be considered. It is also critical to routinely review the patient’s drug regimen to recognise and minimise or discontinue medications that are not effective, no longer required, or that lead to an unnecessary burden of side effects.
Recommendation
APA recommends that patients with schizophrenia be treated with clozapine if the risk for suicide attempts or suicide remains substantial despite other treatments.
Clozapine therapy can be successful in reducing suicidal behaviour if, despite other therapies, the risk remains substantial. Furthermore, clozapine therapy can be effective in reducing the rate of suicide attempts and suicide in people with schizophrenia, irrespective of whether formal requirements for treatment resistance have been met. Although demographic and historical risk factors remain immutable, a variety of other risk factors can theoretically be changed and may function as intervention criteria in the formulation of a treatment plan. As in other conditions where patients do not tend to respond entirely to care, it is important to pay attention to adherence.
Recommendation
APA suggests that patients with schizophrenia be treated with clozapine if the risk for aggressive behavior remains substantial despite other treatments.
Clozapine use may decrease the probability of aggressive behaviour in individuals with schizophrenia who are at significant risk for aggressive behaviour. Higher rates of treatment response are additional benefits of clozapine treatment; decreases in psychotic symptoms, all-cause mortality, overall hospitalisation rates, and discontinuation of treatment due to lack of effectiveness and lower rates of self-harm, suicide attempts, or hospitalizations to prevent suicide. While overall adverse event rates do not vary with clozapine compared to risperidone (low evidence intensity), clozapine has a higher risk of withdrawal from the study due to adverse effects than any other SGAs (low evidence strength of research). Rare but serious consequences, including extreme neutropenia, myocarditis, cardiomyopathy, and NMS, are particular harms associated with clozapine use. Such harms may not be prevented, but the risk of serious neutropenia is reduced by the requisite ANC monitoring. The risk can also be minimised by early exposure to and awareness of NMS and cardiac risks of clozapine use. Clozapine seizures are often more common than other antipsychotics, but can be reduced by gradual titration of the dosage of clozapine, avoidance of extremely high doses of clozapine, and attention to pharmacokinetic factors that could result in rapid changes in the levels of clozapine. Constipation with clozapine and in certain patients with faecal deficiency or paralytic ileus may also be important.
Recommendation
APA suggests that patients receive treatment with a long-acting injectable antipsychotic medication if they prefer such treatment or if they have a history of poor or uncertain adherence.
For patients, families, and physicians, LAI formulations of antipsychotic drugs may have a variety of benefits, but they are often underused. There are also ethnic disparities in the percentage of individuals who are treated with LAI antipsychotic drugs with higher black use of these formulations relative to white patients. There is greater certainty with LAI antipsychotic drugs that a patient can receive treatment on an ongoing basis as there are less chances to skip it.
Recommendation
APA recommends that patients who have acute dystonia associated with antipsychotic therapy be treated with an anticholinergic medication.
The use of medicines with anticholinergic properties (including diphenhydramine, benztropine, and trihexyphenidyl) can be correlated with rapid symptom relief in people who have acute dystonia associated with antipsychotic treatment. In addition, continuation of anticholinergic drug therapy can prevent dystonia from returning before further changes can be made to the treatment plan to reduce the risk of recurrence. Side effects such as dry mouth, blurred vision, precipitation of acute angle glaucoma, constipation (and in some cases faecal impairment), tachycardia, urinary retention, effects on thermoregulation (e.g. hyperthermia in hot weather), reduced learning and memory, slowed cognition, and anticholinergic to acute dystonia include the harms of taking an anticholinergic medication. These harms are likely to be greater in older individuals and may be augmented in individuals taking other medications with anticholinergic properties.
Recommendation
APA suggests the following options for patients who have parkinsonism associated with antipsychotic therapy: lowering the dosage of the antipsychotic medication, switching to another antipsychotic medication, or treating with an anticholinergic medication.
A decrease in signs and symptoms such as rigidity, tremor, and bradykinesia in people who have medication-induced parkinsonism may be of substantial benefit if such a reduction is achieved by lowering the dosage of antipsychotic medication, moving to another antipsychotic medication that is less likely to cause parkinsonism, or using anticholinergic drugs. An rise in psychotic symptoms may be associated with lowering the dosage of an antipsychotic drug or switching to a new antipsychotic medication. Side effects such as dry mouth, blurred vision, precipitation of acute angle-closure glaucoma, constipation (and in some cases faecal impairment), tachycardia, urinary retention, effects on thermoregulation (e.g., hyperthermia in the treatment of drug-induced parkinsonism) are the harms of using a medication with anticholinergic properties. These harms are likely to be greater in older individuals and may be augmented in individuals taking other medications with anticholinergic properties.
Recommendation
APA suggests the following options for patients who have akathisia associated with antipsychotic therapy: lowering the dosage of the antipsychotic medication, switching to another antipsychotic medication, adding a benzodiazepine medication, or adding a beta-adrenergic blocking agent.
In people with antipsychotic drug-related akathisia, reducing symptoms can be of substantial benefit if such a reduction is done by reducing the dosage of antipsychotic medications, moving to another antipsychotic drug that is less likely to induce akathisia, or using a benzodiazepine or a beta-adrenergic blocking agent to treat akathisia. Reducing the dose of an antipsychotic medication or changing to a different antipsychotic medication can be associated with an increase in psychotic symptoms.
Sleepiness, cognitive difficulties, concentration issues, and the possibility of abuse or development of sedative use disorder can be the harms of using a benzodiazepine. Respiratory depression can occur at high doses, especially in combination with alcohol, other sedating medications, or opioids. The primary harm in the use of a beta-adrenergic blocking agent such as propranolol is the reduction in blood pressure.
Recommendation
APA recommends that patients who have moderate to severe or disabling tardive dyskinesia associated with antipsychotic therapy be treated with a reversible inhibitor of the vesicular monoamine transporter2 (VMAT2).
In individuals with moderate to severe or disabling tardive dyskinesia associated with antipsychotic therapy, VMAT2 inhibitors can be associated with significant reductions in motor signs and symptoms of tardive dyskinesia.
Psychosocial Interventions
Recommendation
APA recommends that patients with schizophrenia who are experiencing a first episode of psychosis be treated in a coordinated specialty care program.
Lower mortality, lower relapse rates, improved quality of life, better global function, and greater possibility of working or remaining in school after receiving up to two years of care can be correlated with the use of a CSC programme for individuals with a first episode of psychosis. The harms of a CSC programme are not well delineated for individuals with a first episode of psychosis, but are likely to be minimal.
Recommendation
APA recommends that patients with schizophrenia be treated with cognitive-behavioral therapy for psychosis (CBTp).
The use of CBTp in the treatment of schizophrenia can be associated with an overall decrease in symptoms of the central condition, such as positive symptoms. CBTp may also be correlated with short-term changes in the quality of life and global, social, and occupational functions (e.g. for up to 6 months). The harms of CBTp are not well delineated or routinely examined in the treatment of schizophrenia, but are likely to be small based on the small number of harms documented in clinical trials.
Recommendation
APA recommends that patients with schizophrenia receive psychoeducation.
A variety of possible advantages may be correlated with the use of psycho-education in the treatment of schizophrenia, including changes in global functioning and decreases in relapse rates. In several research, changes in adherence to care and increased satisfaction of mental health services have also been reported. The harms of psychoeducation are likely to be small based on clinical trial findings that indicate little variance in the rate of harms encountered by people treated with psychoeducation.
Recommendation
APA recommends that patients with schizophrenia receive supported employment services.
The use of assisted jobs as part of schizophrenia care can be associated with substantially improved employment outcomes, including a significantly higher likelihood of securing competitive employment, a significantly higher probability of working more than 20 hours per week, more weeks of employment and higher earnings relative to vocational training or no vocational intervention. The harms of supported employment in the treatment of schizophrenia are not well delineated or systematically reported but are likely to be small.
Recommendation
APA recommends that patients with schizophrenia receive assertive community treatment if there is a history of poor engagement with services leading to frequent relapse or social disruption (e.g., homelessness; legal difficulties, including imprisonment).
A variety of advantages compared to care as normal can be correlated with the use of ACT in the treatment of schizophrenia, including a greater chance of being domiciled, living alone or working, and a lower likelihood of being hospitalised. The harms of ACT are not well delineated but are likely to be mild in the treatment of schizophrenia.
Recommendation
APA suggests that patients with schizophrenia who have ongoing contact with family receive family interventions.
The use of family strategies to treat schizophrenia will decrease the risk of relapse and decrease symptoms of the core disorder. The damage to the treatment of schizophrenia by family interventions is not well known, but appears to be limited. Clinical experience shows that many patients agree with family interventions and consider them as part of a treatment plan; but in the past, some patients may have experienced issues in relationships with family members in the past and may not want family members to be involved in their treatment.
Recommendation
APA suggests that patients with schizophrenia receive interventions aimed at developing self-management skills and enhancing person-oriented recovery.
Reductions in symptom severity and risk of relapse and an enhanced sense of optimism and empowerment may be correlated with the use of therapies aimed at improving self-management skills and promoting person-oriented rehabilitation in people with schizophrenia. Self-management techniques aimed at treating co-occurring medical problems in people with significant mental illness often have advantages that include enhanced patient activation and increased quality of life related to health. The harms of self-management skills learning strategies and enhancement of person-oriented rehabilitation in schizophrenia care are not well studied, but are likely to be negligible. Clinical experience shows that the majority of patients cooperate and consider therapies aimed at enhancing skills in self-management and improving person-oriented rehabilitation. However, because of personal preferences or logistical barriers, some patients do not want to take part in such interventions (e.g., transportation, childcare) to attending group sessions.
Recommendation
APA suggests that patients with schizophrenia receive cognitive remediation.
The use of cognitive remediation is associated with modest changes in specific aspects of cognition, as well as minor positive effects on social, occupational and global functioning, symptoms of core disease (low intensity of research evidence), and negative symptoms. In the sense of a person-centered treatment plan that involves evidence-based non-pharmacological and pharmacological therapies for schizophrenia compared with normal care over approximately 16 weeks of treatment, this recommendation statement should be enforced. The harms of cognitive remediation are not well-studied in the treatment of schizophrenia, but are likely to be minimal. Evidence from clinical studies shows that as part of a treatment plan, patients are likely to engage with and consider cognitive remediation; however other patients do not want to participate because of logistical obstacles (e.g. time, expense, transport, childcare).
Recommendation
APA suggests that patients with schizophrenia who have a therapeutic goal of enhanced social functioning receive social skills training.
Use of social skills training in the treatment of schizophrenia can more than normal care, improve social function, core disease symptoms, and negative symptoms. In the treatment of schizophrenia, the damage of social skills training has not been well documented but tends to be limited. Clinical experience shows that as part of a recovery plan, many patients are cooperative with and support social skills training; however, due to logistical obstacles (e.g. time, expense, transportation, child care) or having expectations for treatment that are unrelated to social skills, other patients may not choose to take part in social skills training.
Recommendation
APA suggests that patients with schizophrenia be treated with supportive psychotherapy.
In the treatment of schizophrenia, the use of supportive psychotherapy was not correlated with relative benefits in global or social functions compared to treatment as normal. However, under certain cases, treatment already requires positive psychotherapy as normal. In addition, clinical experience indicates that advantages such as improving the therapeutic relationship, minimising demoralisation, and implementing realistic coping mechanisms in the treatment of individuals with schizophrenia can be correlated with positive psychotherapy. While evidence is minimal, the damage of using supportive psychotherapy in the treatment of schizophrenia appears to be negligible. However, there could be indirect detrimental consequences if positive psychotherapy is used preferentially instead of a treatment, which is correlated with more consistent proof of benefit. Clinical experience shows that most patients, even though they are hesitant to participate in other psychosocial treatments, are cooperative with and consider positive psychotherapy as part of a recovery plan. However certain patients do not want to participate in psychotherapy or may have logistical obstacles that make it difficult to attend psychotherapy sessions (e.g., time, transportation, financial considerations).
Reference:
- Keepers GA, Fochtmann LJ, Anzia JM, Benjamin S, Lyness JM, Mojtabai R, et al; (Systematic Review). The American Psychiatric Association Practice Guideline for the Treatment of Patients With Schizophrenia. Am J Psychiatry. 2020 Sep 1;177(9):868-872.

