Combination Very Low Dose Sulphonylurea and DPP4 Inhibitor have a Potent Glucose Lowering Effect through Augmentation of Beta Cell Function without Increase in Hypoglycaemia
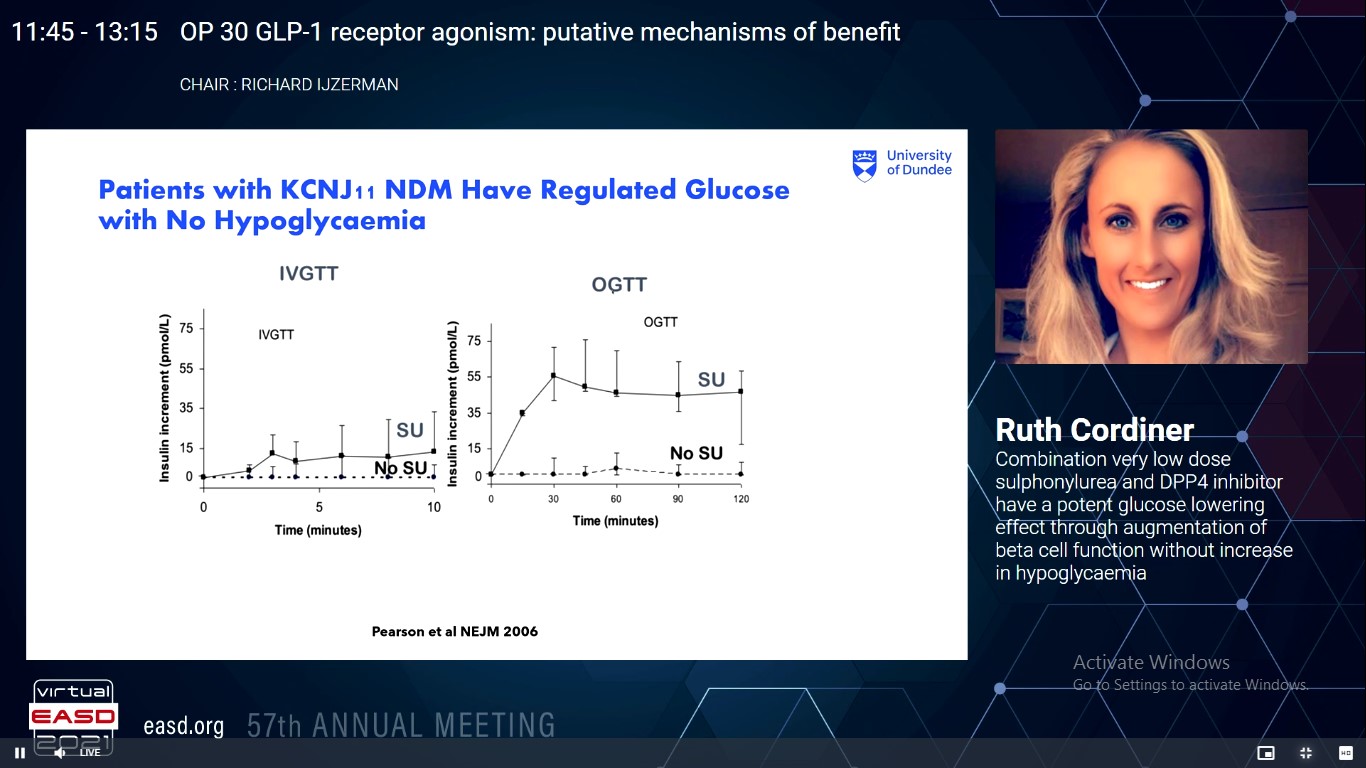
By 2035, the global prevalence of diabetes will surpass 600 million contributed by low and middle-income countries. Low dose use of sulphonylurea can counteract the negative aspects, particularly hypoglycaemia, weight gain and reduced durability. Cordiner RM, presented a study in a session at Virtual EASD Annual Meeting 2021 on 29th September 2021 which hypothesized the potential synergy between low dose SU in combination with a DPP4 inhibitor.
A total of 30 individuals with T2DM (HbA1c <64mmol/l) treated with diet or metformin monotherapy were allocated in a single-centre, open-label, randomised crossover study. Participants completed four, 14-day blocks in a random order: control, gliclazide 20mg once daily (SU), sitagliptin 100mg (DPP4), or combination (SUDPP4). Beta cell function was modelled through the relationship between insulin secretion and glucose concentration. The primary outcomes assessed were the evaluation of treatment on beta cell glucose sensitivity and CGM parameters were assessed as secondary outcomes.
A potent additive glucose lowering effect was shown by linear mixed model estimates mean glucose from area under the curve (mean 95% CI) (mmol/l): Control 11.5 (10.7 – 12.3), DPP4 10.2 (9.4 – 11.1), SU 9.7 (8.9 – 10.5), SUDPP4 8.7 (7.9 – 9.5) (p <0.001) which was mirrored by the glucose sensitivity.
A progressive increase in insulin secretion at the same glucose concentrations (i.e. increased glucose sensitivity) in favour of combination DPP4 and SU was observed.
These results suggest that combination low dose gliclazide with a DPP4 inhibitor shows potent glucose lowering effect and glucose reduction was achieved at gliclazide concentrations far below those achieved with standard therapeutic doses (~600ng/ml vs >5000ng/ml Cmax with 80mg gliclazide daily).
Impact of the Fasting Plasma Glucose Titration Target on the Success of Basal Insulin Titration in Insulin-naive Patients with Type 2 Diabetes: A Systematic Analysis

The algorithms of basal insulin titration differ in their fasting plasma glucose (FPG) targets. Wolters J, presented a study in a session at Virtual EASD Annual Meeting 2021 on 29th September 2021 which compared beneficial (glycaemic control) and adverse outcomes (hypoglycaemia, weight gain) of basal insulin titration carried out with FPG titration targets (TT).
A total of 42 publications reporting clinical trials were retrieved from PubMed literature search in 17643 insulin-naïve patients with type 2 diabetes. 61 individual study groups were divided as per FPG TT (a: ≤ 5.0; b: 5.01-5.6; c: ≥ 5.61 mmol/l). Weighted means and their standard deviations were calculated for: FPG, HbA1c, target achievement, incidence of any or severe hypoglycaemic events, and insulin doses.
After titration, i.e. at the study end, achieved FPG and HbA1c were lower with more ambitious titration targets (a. 6.17 [6.11; 6.24]; b. 6.67 [6.63; 6.71]; c. 6.93 [6.79; 7.06] mmol/l and a. 7.08 [7.05; 7.11]; b. 7.19 [7.18; 7.21]; c. 7.32 [7.26; 7.37] %; p < 0.01 for all comparisons).
- In FPG TT a, HbA1c target achievement (≤ 7.0 or 6.5 %) was highest, intermediate with b, and worst with c (p <0.01).
- In subgroup a, the basal insulin dose achievement was highest
- With lower FPG TTs, the incidence of (severe or any) hypoglycaemic episodes was not higher
- Body weight gain (1 to 2 kg across all subgroups) was not more prominent as well.
Improvement in glycaemic control can be achieved by aiming for a lower FPG titration target without increasing the risk for adverse events like hypoglycaemia or increased body weight.
Indirect Effect of COVID Pandemic on Cardiovascular Hospitalisations
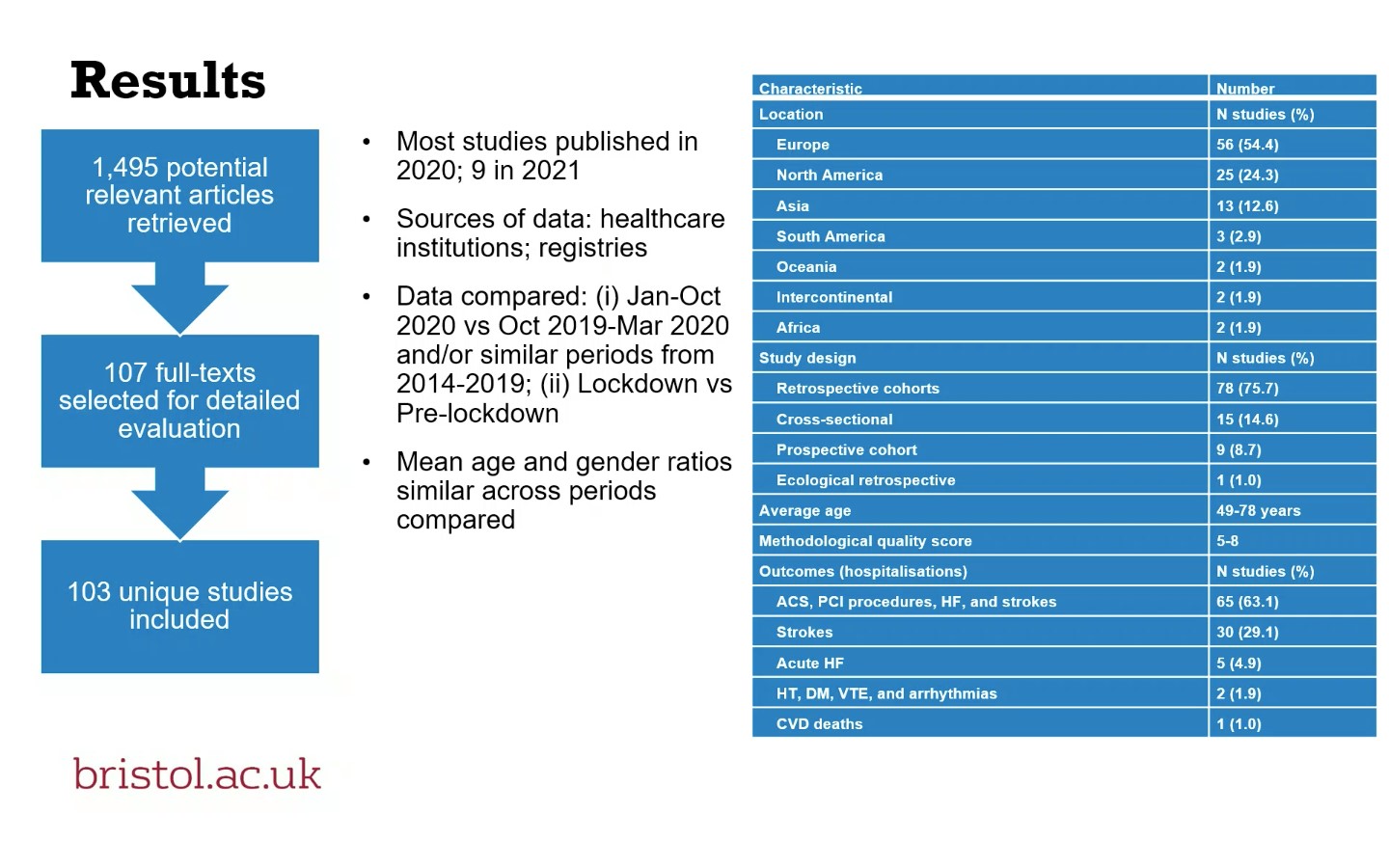
Kunutsor S, presented a session on “Indirect effect of COVID pandemic on cardiovascular hospitalisations” at Virtual EASD Annual Meeting 2021 on 30th September 2021.
A study was conducted to assess the indirect impact of the COVID-19 pandemic on hospitalisations for and the management of cardiometabolic conditions. The study was conducted according to a predefined protocol and PRISMA and MOOSE guidelines. All clinical observational studies were included. These studies evaluated indirect impact of COVID-19 on hospitalisations for cardiometabolic conditions and their management. The studies reported comparisons between the pandemic period vs. pre-pandemic and/or historical period. Most studies published in 2020 and 2021 were included. Except for 12 studies, all reported decline in hospitalisations comparing pandemic with pre-pandemic periods (ranging from 20.2 to 73.0%). Eleven of 12 studies reported no increase or no changes in stroke hospitalisations. The severity of presentation was reported by 26 studies. Measures of severity were assessed by increase in levels of cardiac enzymes, worsened left ventricular ejection fraction (LVEF), higher NIHSS score. Most studies reported severe presentation during pandemic compared with pre-pandemic period. 36 studies reported data on procedures performed in hospital. The procedures included coronary angiography, PCI, thrombolysis, MRI, acute revascularisation. Most studies reported less procedures being performed during pandemic compared with pre-pandemic period. Fifty-five studies reported on delays during presentation and management. Delays reported were time between symptom onset to first medical contact, emergency transport, and consultation-intervention. Most studies reported more delays during pandemic compared with pre-pandemic periods. Most common patient delay was time between symptom onset and first medical contact. The reasons cited for delays in seeking medical care were fear of contracting COVID-19 which added extra burden to healthcare system. Most studies reported a shorter length of stay during pandemic compared with pre-pandemic (1-8 vs. 2-12 days). Most studies reported no change in in-hospital mortality or discharge disposition during pandemic compared with pre-pandemic period. Twenty-three studies reported an increase in worse in-hospital outcomes.
This was a real world study gathering data across 6 continents. Health-seeking behaviour of patients for acute cardiometabolic conditions, their management, and outcomes have all been adversely impacted by the COVID-19 pandemic. Despite this, in-hospital deaths were not significantly affected.
Several potential reasons for the decline in hospitalisations increased severity on presentation and delays in management. Despite the delays, change in the in-hospital mortality suggested care for patients was not compromised. Implications for cardiovascular care are needed. It is important to prepare for future pandemics and educate patients.
Prediabetes: Innocent or Guilty? Insights from the Maastricht Study
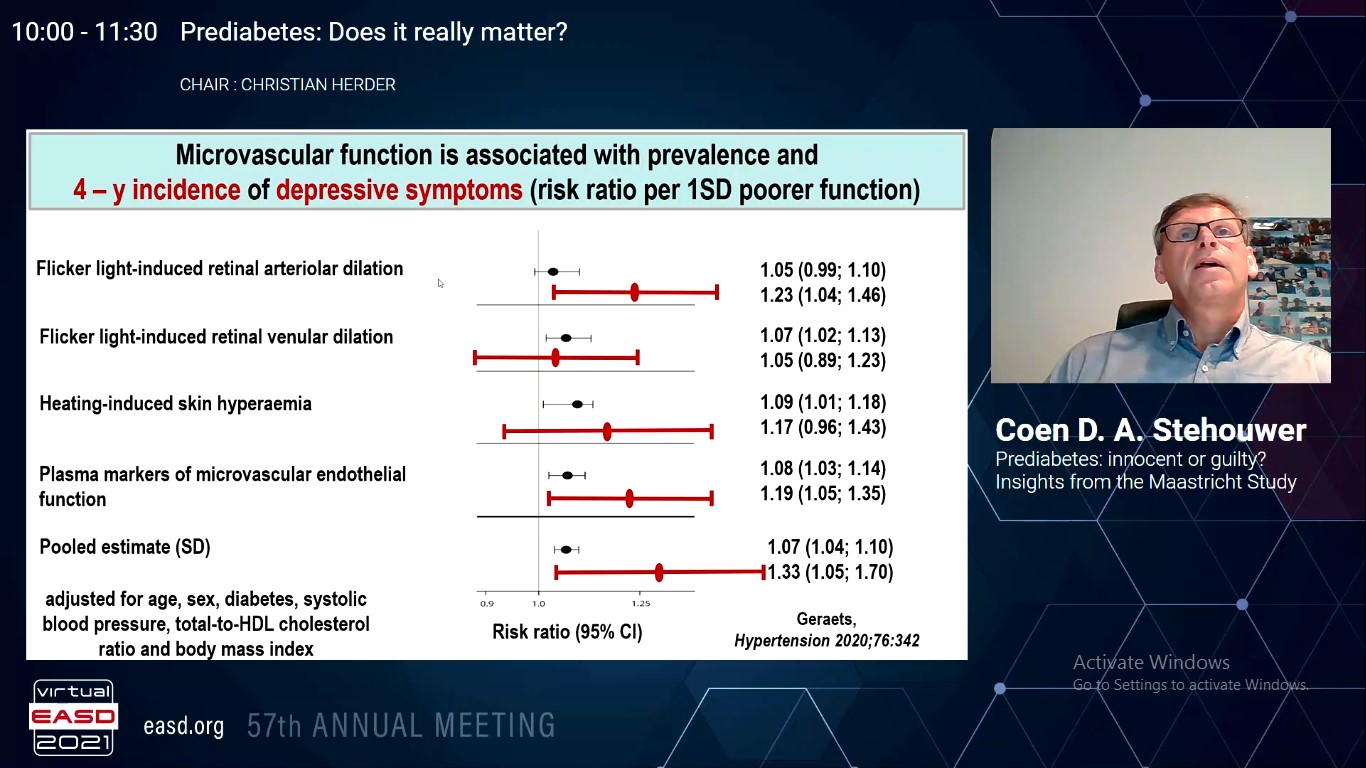
Stehouwer CDA, presented a session on “Prediabetes: Innocent or Guilty? Insights from the Maastricht Study” at Virtual EASD Annual Meeting 2021 on 29th September 2021.
Prediabetes is simply early diabetes and its charge is in terms of its consequences. Prediabetes strongly varies with BMI and age. It occurs at ~25% among 40-75 year old while at age 60, is ~5% if BMI <25 and ~40% if BMI is ≥35. Many studies have evidence that diabetes is strongly correlated with cardiovascular death and supportive evidence from mandelian randomization showed positive association between genetically proxied HbA1c and CHD in non-diabetic people. Diabetes has relevance with comorbidities such as retinopathy, kidney disease, and neuropathy. Also, stroke, dementia, depression, heart failure and even T2DM itself. HbA1c and prediabetes are associated with retinal arteriolar and venular diameters in retinopathy. Vasodilation in retina and skin is impaired in T2D and prediabetes. It is measured with analysis of retinal dynamic vessel and skin laser Doppler flowmetry. In T2D, cerebral white matter hyperintensities (WMH) and volume loss increases are linked to cerebral vessel disease. All the three parameters HbA1c, FPG and 2hPG are related with WMH. cerebral vessel disease predisposes to stroke, cognitive impairment depression. Microvascular function of body is associated with prevalence and 4-y incidence of depressive symptoms. Hyperglycemia is toxin for endothelial and neural cells leads to neuronal dysfunction and neurogeneration. T2D and prediabetes are associated with thinning in corneal and retinal nerve fiber length. Retinal neurodegeneration is associated with brain atrophy and also 7-year incidence of depressive symptoms. The studies exhibited that glucose intolerance and diabetes showed strong correlation with CVD events and microvascular disease. Treatment of prediabetes is necessary to prevent or delay the progression of diabetes.
Diabetes is a progressive macrovascular, microvascular and neuronal disorder that affects many organs and that starts in prediabetes.
Cardiovascular Risk in Prediabetes

Faerch K, presented a session on “Cardiovascular Risk in Prediabetes” at Virtual EASD Annual Meeting 2021 on 29th September 2021.
A prospective study of 22 groups in Europe showed that cardiovascular disease (CVD) is leading factor in mortality in prediabetes patients. The 2H-BG is a better predictor of deaths from all causes and CVD than in FBG with significant difference in rise of impaired glucose tolerance (IGT) and normal glucose tolerance (NGT). According to WHO and ADA, people with IFG and IGT exhibited ~20% increased risk of CVD as compared to their normoglycemic counterparts. The risk can be reduced by ~50% following adjustment for conventional CVD risk factors. FPG is modest and 2h-BG is good predictor of CVD but both had high variability.
In the use of HbA1c to diagnose diabetes and high risk patients, the categorical clinical states pre-diabetes, IFG, and IGT fail to capture the continuum of risk and will be phased out of use as HbA1c measurements replace glucose measurements. As per the ADAG study, less than 40% variance in Hba1c could be explained in people without diabetes. HbA1c is affected by anaemia, iron deficiency, genetics, etc. There was >20% increased risk of CVD was seen in people with prediabetes diagnosed by HbA1c compared to their normoglycemic counterparts .No difference in survival rate was seen between prediabetes and normoglycemic groups after adjusting for previous CVD, soking, TC, HDL-C, SBP. HbA1c is very good predictor of CVD. It is convenient for patients and also accurate and precise. The near 2-fold higher unadjusted risk for CVD in people with prediabetes is driven mainly by abnormal levels of conventional CVD risk factors.
Prediabetes is associated with 20% increased risk of CVD compared to normoglycemic individuals. But, ~50% of the risk is driven by conventional non-glycemic CVD risk factors. Prediabetes is not one entity with different diagnostic criteria and different pathophysiology. A balance between feasibility and convenience on one hand and scientific data on the other hand is needed. The focus should be on developing risk scores for the population without diabetes to target individual at the highest risk of CVD, not only focus on glycemia (prediabetes) using arbitrary cutpoints.
Validation of the Classification for Type 2 Diabetes into Five Subgroups: A Report from the ORIGIN Trial
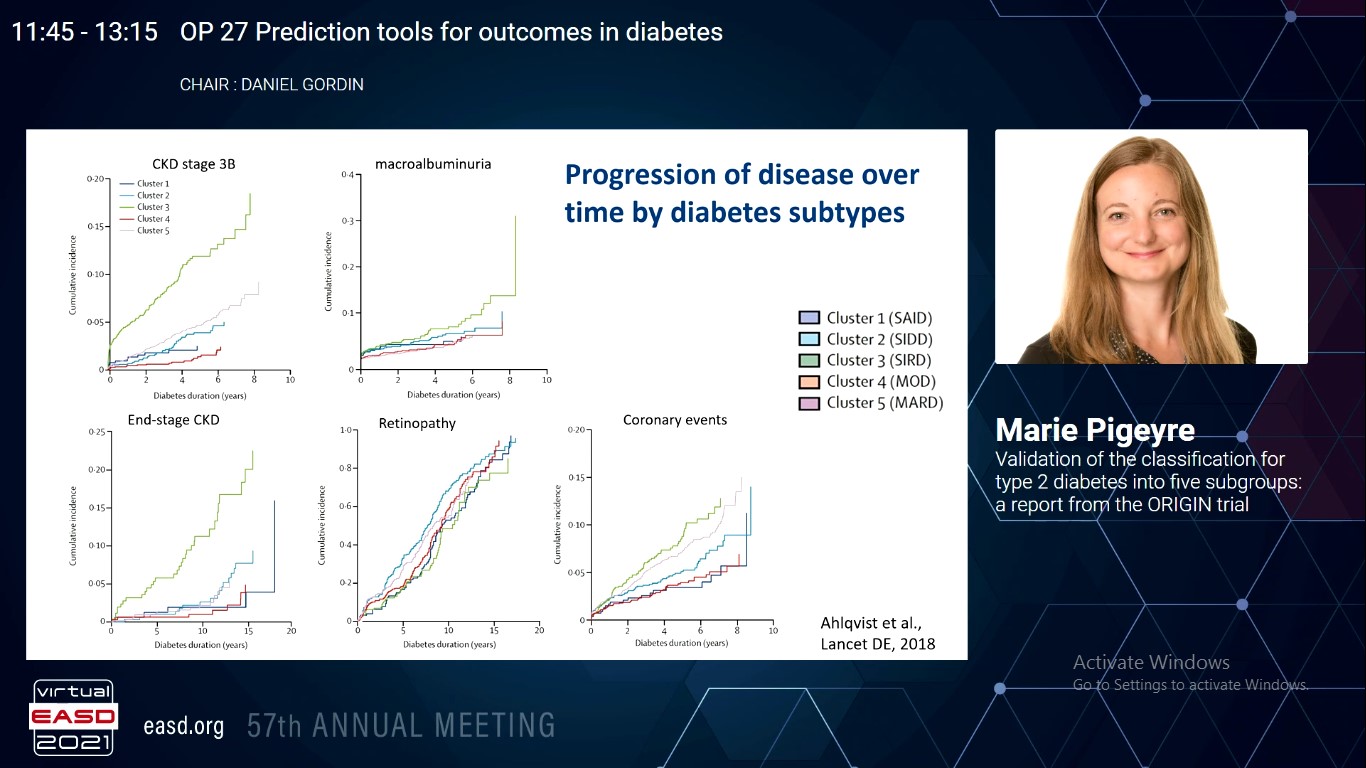
It has been observed that diabetes could be segregated into five subtypes as per the progression of dysglycemia and the incidence of diabetes consequences which has been found in Swedish individuals with newly diagnosed diabetes. Pigeyre M, presented a study in a session at Virtual EASD Annual Meeting 2021 on 29th September 2021.
A total of 7,017 participants from the Outcome Reduction with Initial Glargine Intervention (ORIGIN) trial were allocated in five predefined diabetes subtypes (namely, severe auto-immune diabetes (SAID), severe insulin-deficient diabetes (SIDD), severe insulin-resistant diabetes (SIRD), mild obesity-related diabetes (MOD), mild age-related diabetes (MARD)). This allocation was done on the basis of: age at diabetes diagnosis, body mass index, glycosylated haemoglobin, fasting C-peptide levels, and presence of glutamate decarboxylase antibodies at baseline.
Difference of cardiovascular and renal outcomes in different subtypes were assessed using Cox regression models for a median follow up of 6.2 years and comparison was done between of glargine versus standard care on hyperglycemia. These five different subtypes were replicated in the ORIGIN trial and similar characteristics were found in Europeans and Latin Americans, in comparison to the initially described clusters in the Swedish cohort. A significant difference was found in the renal outcome, with higher incidence of events in SIRD compared to the MARD subtype (i.e., chronic kidney disease stage 3A: HR=1.47, 95%CI [1.30-1.67]; stage 3B: HR=2.20 [1.80-2.69]; macroalbuminuria: HR=1.48 [1.17-1.86]). After the adjustment for multiple hypothesis testing, no differences were found in incidence of retinopathy and cardiovascular diseases. However, these different diabetes subtypes showed different glycaemic response to glargine in the SIDD subtype compared to the MARD subtype, with a decreased risk of hyperglycemia by 14% (OR=1.37 [1.32-1.43] on glargine; OR=1.51 [1.45-1.58] on standard care;
Characterization of five different diabetes subtypes in a multi-ethnic cohort was enabled by cluster analysis. The incidence of renal events and response to insulin was different between diabetes sub-types. These results suggest the use of precision medicine to predict co-morbidities and treatment responses.
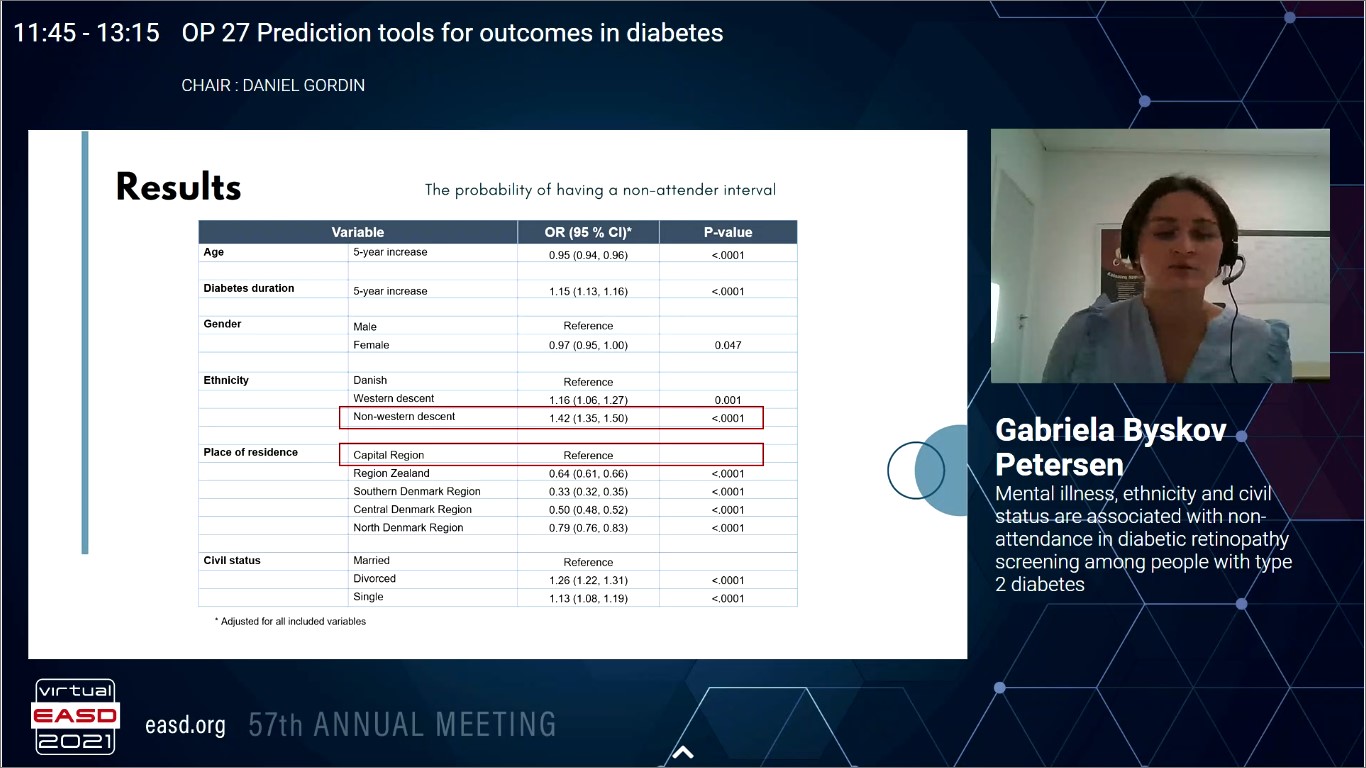
Mental illness, Ethnicity and Civil Status Are Associated with Non-attendance in Diabetic Retinopathy Screening Among People with Type 2 Diabetes
Diabetic retinopathy can results in serious vision loss and blindness, if not managed properly. But, the participation in eye screening is below recommended levels. Petersen GB, presented a study in a session at Virtual EASD Annual Meeting 2021 on 29th September 2021 which analysed the factors with non-attendance in screening for diabetic retinopathy in people with type 2 diabetes.
Individual register data from 156,878 people with type 2 diabetes aged 40-70 years was collected in this retrospective, observational study. Each individual was categorised as an attender (at least one registered screening) or a never-attender (no registered screening) on the basis of eye screening history from 2013 till 2018. Baseline characteristics were compared between attender and non-attender using non-parametric tests including Age, Gender, Ethnicity, Place of residence (region), Civil status, Education, Employment, Income, Diabetes duration and Comorbidity and mental health.
In the attenders, 230,173 screening intervals were analysed and if the person failed to participate in the eye screening within the recommended interval, it was defined as non-attender intervals. About 27% of individuals were recognized as non-attenders, having no registered eye screening. The comparison parameters exhibited that attenders and non-attenders differed significantly on all baseline characteristics. Never-attenders were more frequently divorced, 30% vs. 22% (p<.0001), living in the Capital Region, 36% vs. 28% (p<.0001), mentally ill 10% vs. 5% (p<.0001) and had more comorbidities, 22 % vs. 17 % (p<.0001) as compared to attenders.
This is the first national study which focuses the non-attendance in people with type 2 diabetes for diabetic retinopathy. The findings of the study showed that both never-attendance and non-attendance are frequent in people who are divorced and among people of poorer health. Furthermore, non-attendance is more common between people of non-western decent.

